


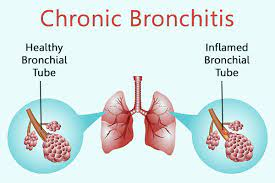
CHRONIC BRONCHITIS
DEFINITION
• Chronic bronchitis is defined as a condition associated with excessive tracheobronchial mucus production to cause cough with expectoration for at least 3 months of the year, for more than 2 consecutive years.
Incidence
• Middle and late adult life. • More in males than in females. • More in smokers than in non-smokers. • More in urban than in rural dwellers.
AETIOLOGY (risk factors)
• Cigarette smoking is the most important risk factor for the development of COPD.
• Air pollution with dust, smoke and fumes, sulphur dioxide and particulate matter. Indoor air pollution, especially from burning biomass fuels (wood, animal dung and crop residues) and coal in confined spaces is associated with increased risk of COPD.
• Occupational hazards as with exposure to dust, smoke and fumes, toluene diisocyanate in plastic industry and carding room workers in cotton mills.
• Familial and genetic factors influence the development of chronic bronchitis:
• Genetic predisposition.
• Children of smoking parents.
• Passive smoking (also known as environmental tobacco smoke).
• Natural gas used for cooking.
• Previous tuberculosis
• Low socio-economic status.
• Pre-existing asthma may be a risk factor.
• Infections with rhinovirus, S. pneumoniae, H. influenzae and can cause exacerbations of chronic bronchitis.
• Exposure to dampness, fog and sudden changes in temperature can cause exacerbations of chronic bronchitis.
CLINICAL FEATURES
History
• The most striking features are an impressive history of cough with sputum production for many years and a relatively late onset of breathlessness.
• Initially, the cough is present only in the winter seasons ("winter cough" or "smoker's cough"), especially in the mornings ("morning cough"). Over years, cough increases in frequency, severity and duration until it is present all around the year.
• The sputum is usually scanty, mucoid and more in the mornings. Sputum is occasionally blood-stained (haemoptysis) and occasionally frankly purulent ("mucopurulent relapse").
• Breathlessness is relatively late in onset in chronic bronchitis. It is due to airflow obstruction and is aggravated by infection, excessive smoking and adverse atmospheric conditions.
• Other symptoms include fever during mucopurulent relapses, wheezing and tightness in the chest.
Physical Signs
• Usually the patient is overweight. • At rest, there is no respiratory distress. Respiratory rate is normal and accessory muscles of respiration are not acting. • Percussion note is normally resonant over the lungs. Liver dullness and cardiac dullness are normal in position.
Auscultation
• Vesicular breath sounds with prolonged expiration. • Inspiratory and expiratory rhonchi.
• Crepitations that either disappear or change in location and intensity after coughing.
Systemic Features
• Decreased free-fat mass. • Impaired systemic muscle function and muscle wasting. • Anaemia. •Osteoporosis. • Depression. • Increased risk of angina, acute myocardial infarction and heart failure. • Metabolic syndrome.
Investigations
• Radiological examination:- Chest radiograph does not show any characteristic abnormality in chronic bronchitis. • Electrocardiography. • Pulmonary function tests. • ABG studies
• Exercise testing:
• Six-minute walk test used to assess disability and effectiveness of pulmonary rehabilitation.
Course and Prognosis (Natural History)
• Chronic bronchitis is a progressive disease characterised by exacerbations and remissions.
• Eventually leads to respiratory and cardiac failure (cor pulmonale).
• Repeated episodes of respiratory and cardiac failure occur, from which prompt recovery occurs with proper treatment.
• Some patients may survive for a few years, while others for many years.
Management
• Regular exercises and nutritional management. • Weight loss in obese patients. • Reduction of bronchial irritation- Stop smoking completely. Dusty and smoke-laden atmospheres should be avoided. • Treatment and prevention of respiratory infections. • Vaccination with pneumococcal and influenza vaccines.
• Symptomatic measures- Hot drinks or steam inhalations to liquefy sputum and Chest physiotherapy. • Long-term domiciliary oxygen therapy. • Pulmonary rehabilitation:- It includes breathing techniques, chest physical therapy, postural drainage, exercise conditioning (upper and lower extremity) and activities of daily living. Also included are evaluation and advice on nutritional needs and psychological and vocational counselling.
TREATMENT AT DR. SOHAN LAL CLINIC
The integrated POLYCLINIC facility offers patients to select their treatment either from the Department of Homeopathy or from the Department of Medicine.
We provide scientific, research-based, and professional services to people across the world, aiming to achieve the highest success rate.
